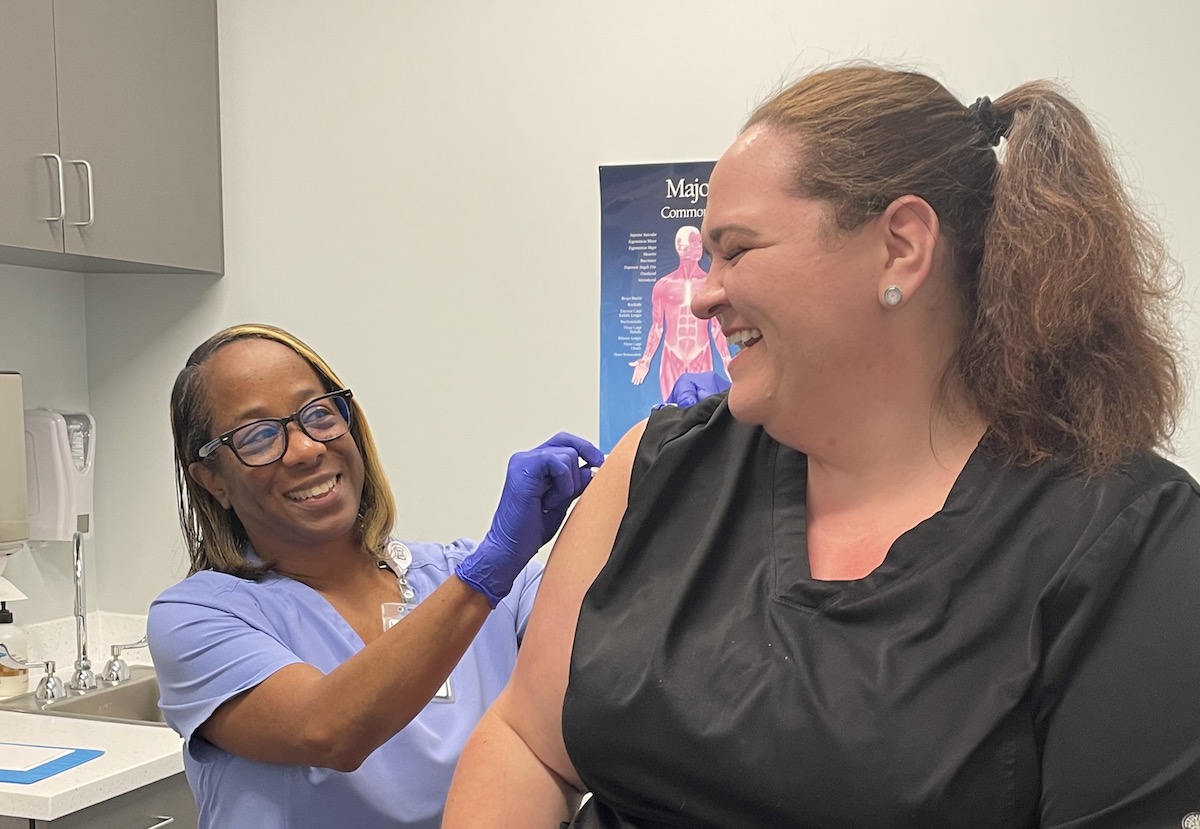
Tryon registered medical assistant Donna Ferguson (right) administers a vaccine to patient services specialist Brooke Knudson (left) to help her avoid serious illness during the 2023 upper respiratory virus season.
While fall brings the leaves changing colors, apple picking and all things pumpkin, it also begins the season of respiratory illness. Colder temperatures leading to more time spent inside, school and holiday travel all help contribute to this uptick. Thankfully, new vaccines are available for COVID-19 and flu and, for the first time, there is an RSV vaccine for high-risk populations ages 60+. Tryon Medical Partners internal medicine physicians Kym Furney, MD, and G. Ryan Shelton, MD, are here to answer your vaccine questions and help you get prepared (and protected) for the months ahead.
Is the new COVID vaccine different from previous boosters?
The new COVID vaccine is actually not a booster at all but, rather, a brand new shot.
“A booster is a reminder of what you had previously, while this latest vaccine has been reformulated to cover the strain that is most commonly circulating,” says Dr. Ryan Shelton. “COVID keeps changing, that’s what viruses do. We have to evolve with it and the new vaccine is an update.”
Another way to remember that the new COVID vaccine is not a booster is to think about the annual flu shot. We don’t refer to the flu shot as a flu booster, since we know the vaccine is reformulated each year to match the expected strain.
I’ve already been vaccinated against COVID. Do I really need the new vaccine?
The short answer is yes. Since the vaccine has been reformulated to target the current variants, it will provide the most protection against serious disease from COVID.
“COVID vaccinations from the spring and earlier are not likely to be effective against the current circulating strain,” shares Dr. Kym Furney. “And as we know, protection from a prior COVID infection or vaccine only lasts a certain amount of time and it’s been a while since most people were last vaccinated.”
What if I’ve never been vaccinated for COVID before? Can I start with this new vaccine?
Yes! Those six years of age and older will be considered up to date after one dose of the new COVID vaccine.
I’ve recently had COVID. Do I still need the new vaccine or is natural immunity enough?
It is important to stay up-to-date with current vaccinations. The CDC recommends waiting three months after a COVID infection to receive the vaccine. And some evidence supports waiting up to six months after infection to be vaccinated.
Those who may have recently received the bivalent booster of the vaccine should wait at least two months before getting the new COVID vaccine.
I’m getting over a cold. When can I get the COVID vaccine?
If you have a mild cold and feel up to it, you can get your COVID shot. However, many symptoms of the common cold mirror COVID symptoms so you want to be sure that you do not actually have COVID (since you need to wait at least three months between infection and the vaccine). The other point to consider is that if your body is already fighting a cold, it may not mount the ideal immune response in processing the vaccine. All this to say that it probably makes sense to give your body a chance to fully recover from any illness before getting vaccinated, unless it is truly a minor cold and you otherwise feel healthy.
Are the new COVID variants circulating now more dangerous?
The good news is that the current strain EG.5 (nicknamed for Eris, the Greek goddess of strife and discord) does not appear to have increased severity of symptoms, still presenting predominantly in the upper respiratory tract with very sore throat and nasal congestion. As with omicron, there has been much less lower respiratory tract disease. The not-so-great news is that Eris does seem to be more transmissible.
Can at-home tests detect Eris? Does Paxlovid still work?
Experts state that home COVID tests should be able to detect Eris. But Dr. Furney reminds us that timing with testing is everything.
“If you have classic symptoms, like large amounts of nasal congestion, sore throat, body aches and your COVID test is negative, you should repeat the test 24 hours later,” she shares. “Testing too early will result in a negative result, when you may very well have COVID that doesn’t show up on an initial test.”
Paxlovid should still be effective against Eris, for high-risk patients or those with a high fever or symptoms of lower tract disease. Paxlovid is a prescription medication and is prescribed by your physician when appropriate.
Why should I get a flu shot? And when?
Simply put, the flu can be very dangerous. The 2022-2023 flu season accounted for 650,000 hospitalizations and 58,000 deaths. The flu vaccine, reformulated each year to match the expected strain, helps protect against infection.
Dr. Shelton says that the goal of the flu vaccine is to significantly decrease any symptoms and lessen the burden of infection. “If you are to get the flu, being vaccinated should make it much milder, easier to weather and less likely to need hospitalization or some of the other more intense treatments.”
It’s never too late to get the flu vaccine, although Dr. Shelton recommends October as the ideal time, so it can last the whole flu season.
Can I get the COVID and flu shots at the same time?
There seems to be no difference in immune response if you get the vaccines at the same time. For most people, it is more convenient to get them together, and doing so ensures that it won’t be put off or forgotten.
I keep hearing about a new shot for RSV. What is RSV and who should get the vaccine?
Respiratory syncytial virus, most commonly referred to as RSV, is a highly contagious common respiratory illness that causes infection in the lungs and breathing passages. This seasonal virus typically begins in falls and peaks in winter. With symptoms similar to a cold, most people recover within one to two weeks. But for infants and older adults, it can be a very serious illness. Each year, it accounts for 60,000-120,000 hospitalizations and 6,000-10,000 deaths for those ages 65+, according to the U.S. Centers for Disease Control and Prevention.
There is now an RSV vaccine available for adults ages 60+ who may be at higher risk for infection. Speak with your clinician to determine if this shot would be beneficial to you. And while you can get the COVID and flu vaccines at the same time, research is less clear about getting the RSV vaccine with others, since it’s a brand new vaccine. For this reason, you may want to wait two to three weeks after getting the COVID and flu vaccines before getting vaccinated against RSV.
Still have questions about COVID, flu or RSV vaccines? Make an appointment with an internal medicine physician.


